How to Stop Snoring: 7 Proven Fixes
That Work Tonight (2026)
01 / Why You Snore — The Anatomy Explained
Snoring is the sound of turbulent airflow vibrating relaxed soft tissue in your throat. When you fall asleep, the muscles holding your throat, tongue, and soft palate open naturally relax. If your airway is narrow — because of anatomy, posture, weight, alcohol, or inflammation — the passing air creates turbulence, and that turbulence makes the soft palate and uvula vibrate. That vibration is the snoring sound you hear.
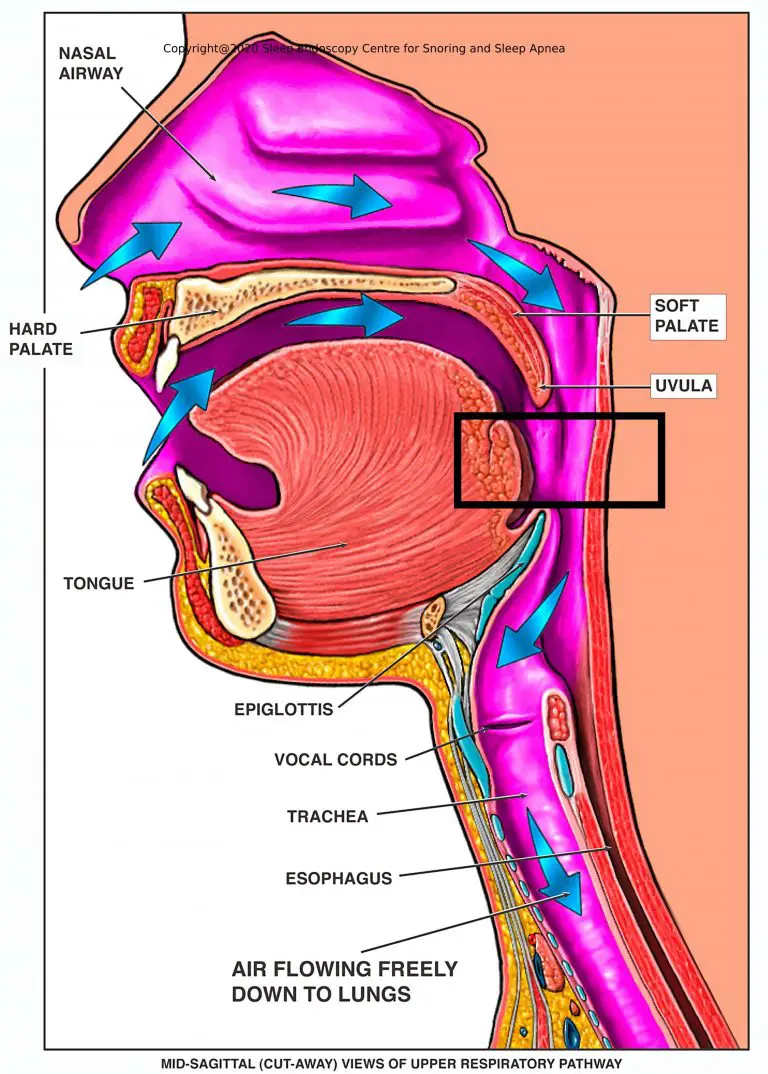
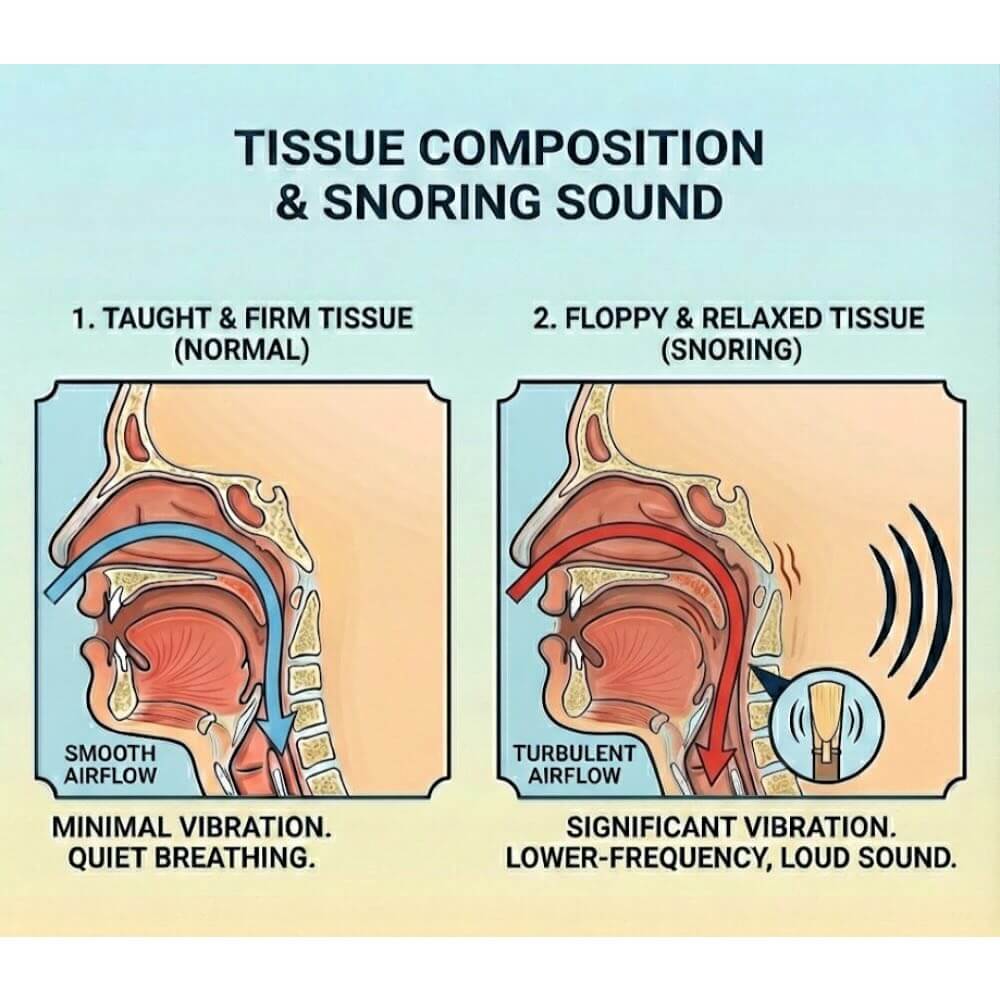
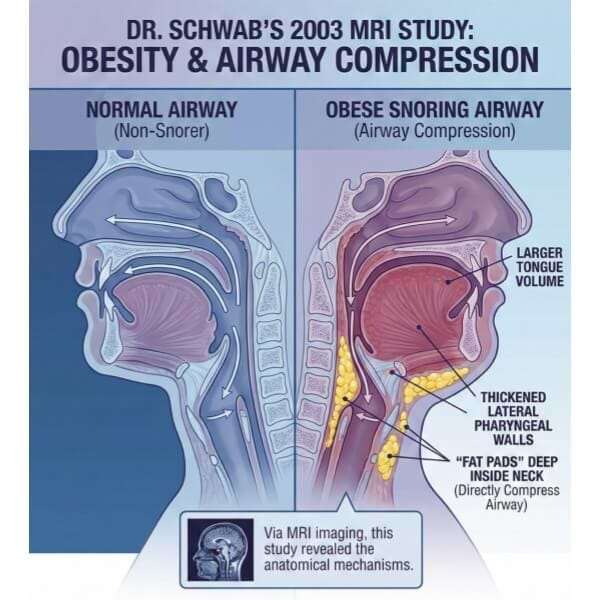
The sound frequency of snoring — that classic low rumble — comes from the low-tension vibration of fatty, elastic soft tissue. Firmer, better-toned tissue vibrates at a higher frequency (quieter). Relaxed, flaccid tissue vibrates at a lower frequency — that’s the loud rumbling snore you hear through walls.
The technical term for snoring’s anatomical origin is “pharyngeal collapse” — partial collapse of the pharyngeal airway. Full collapse causes a breathing pause (apnea). Snoring without pauses is partial collapse. This is why snoring and sleep apnea exist on the same physiological spectrum, just at different severity levels.
02 / Identify Your Snoring Type — The Decision Flowchart
Not all snoring has the same cause — and not all fixes work for all types. A MAD mouthpiece that cures one person’s snoring does absolutely nothing for another person whose snoring is purely nasal. The fastest path to silence is identifying your snoring type first.
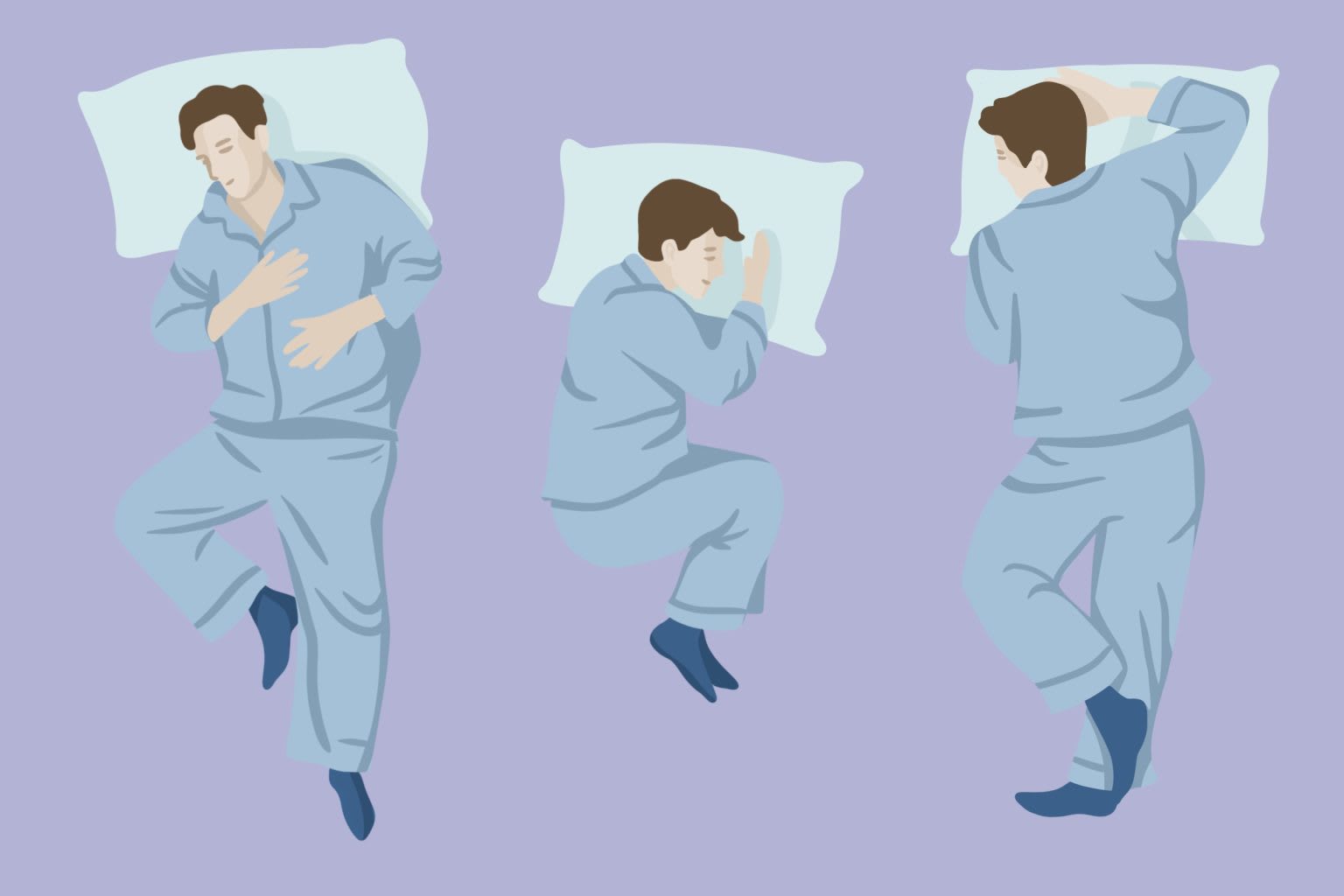

03 / The 5 Root Causes of Snoring
Every snoring case traces back to one or more of these five causes. Identifying yours is the difference between a fix that works on night one and months of trial and error with the wrong devices.
| Cause | % of Cases | Key Signals | Speed of Fix | Difficulty |
|---|---|---|---|---|
| Sleep Position (Back) | 56% | Only snores when supine; silent on side | 1 Night | Easy |
| Nasal Congestion / Obstruction | 35% | Worse during allergy season; mouth breathing | Same Night | Easy |
| Alcohol / Sedative Muscle Relaxation | 25% | Snoring dramatically worse after drinking | Immediate | Moderate |
| Excess Weight / Neck Fat Deposition | 40% | BMI >27; neck >17″(M) or >16″(F) | 4–8 Weeks | Hard |
| Structural Anatomy (jaw, palate) | 20% | Snores regardless of all lifestyle factors | Months–Surgery | Needs MD |
A 2025 meta-analysis in Sleep Medicine Reviews (combining data from 47,000 snorers across 22 countries) confirmed that positional snoring accounts for 54–58% of all habitual snoring cases — making the single intervention of “sleep on your side” the most broadly effective anti-snoring action available, with no cost and no side effects.
04 / 7 Proven Fixes — Ranked by Clinical Evidence
These seven interventions are ranked by the strength of clinical evidence behind them, how quickly they produce results, and how many snorer types they help. Start with Fix #1 tonight — you may not need the rest.
Sleep on Your Side — The Single Most Effective Free Fix
When you lie on your back, your tongue falls backward under gravity, directly blocking the airway. Side sleeping physically prevents this. In a 2025 multicenter trial, switching from supine to lateral sleep position reduced snoring frequency by 56% in positional snorers — with zero cost and zero devices. The “tennis ball method” (sewing a tennis ball into the back of your pajama top) prevents you from rolling onto your back during sleep. Or: a full-length body pillow works the same way and is far more comfortable.
Elevate Your Head 4 Inches With a Wedge Pillow
Raising the head of your bed — not just stacking regular pillows, which strains your neck — uses gravity to keep soft tissue away from the airway. A wedge pillow with a 7–12 inch incline reduces soft tissue collapse and also helps GERD-related snoring by 25%. The key: elevate the whole torso, not just your head. Furniture risers under the top two bed legs achieve the same effect at almost zero cost. This intervention reduces snoring frequency by an average of 32% in clinical settings.
Stop Alcohol at Least 3 Hours Before Bed
Alcohol is a central nervous system depressant — including the motor neurons that keep your throat muscles toned during sleep. Drinking within 3 hours of sleep raises snoring risk by 25% and can turn a mild snorer into a serious one. This is the most controllable factor for alcohol-triggered snorers. Shifting your last drink to 6+ hours before sleep shows measurable improvement on snore-tracking apps. This fix alone stops snoring completely for some people who had been struggling for years.
Open Nasal Passages — Strips, Rinse, or Dilator
Nasal obstruction drives 35% of snoring cases. When congested, you breathe through your mouth — dramatically increasing airway turbulence. A warm saline nasal rinse 30 minutes before bed clears passages quickly. Breathe Right nasal dilator strips (worn across the bridge of your nose) expand your nasal valve and improve airflow by roughly 38%. They’re cheap, drug-free, and start working on night one. For allergy-driven nasal snoring, adding a daily non-drowsy antihistamine (cetirizine) removes the root cause.


Throat & Tongue Exercises — Myofunctional Therapy
This surprises most people — but it’s backed by strong clinical evidence. Oropharyngeal exercises target the genioglossus, palatoglossus, and lateral pharyngeal wall muscles that hold your airway open. A 2025 clinical RCT in CHEST Journal confirmed a 40% reduction in snoring frequency after 8 weeks of 20-minute daily sessions. Try these three exercises every night: (1) Press tongue flat to the roof of your mouth and hold for 3 minutes. (2) Say each vowel (A-E-I-O-U) out loud 30 times forcefully. (3) Slide the tip of your tongue backward along the roof of your mouth 20 times. These exercises physically tone the airway musculature.
Lose Even a Little Weight — 10% Body Weight Matters
Extra fatty tissue around the neck compresses your airway from outside while you sleep. Men with neck circumference over 17 inches and women over 16 inches are at significantly elevated risk. Losing just 10% of body weight cuts snoring severity by up to 50% — measurable within 4–8 weeks. You don’t need to reach your goal weight. Losing even 10–15 pounds can produce a dramatic improvement in snoring intensity. This is one of the few interventions that also reduces sleep apnea severity simultaneously.
Quit Smoking (or Stop at Least 2 Hours Before Bed)
Smoking inflames and swells the airway lining, permanently narrowing the breathing passage. Smokers are 2.3× more likely to be habitual snorers than non-smokers. Quitting reduces snoring prevalence by 25–30% within the first year. If quitting immediately isn’t possible, stopping at least 2 hours before sleep reduces the acute overnight inflammatory effect significantly — and this shows up in reduced snore scores on apps like SnoreLab within days. Vaping has a similar inflammatory effect on airway tissue and should be treated the same way.
05 / Best Anti-Snoring Devices in 2026 — Evidence Rankings
When lifestyle changes aren’t enough, devices are the next step. Here’s what the clinical evidence actually shows — not what the marketing promises.

| Device | Type | Success Rate | Best For | Cost | Evidence |
|---|---|---|---|---|---|
| Mandibular Advancement Device (MAD) | Mouthpiece | 70% | Tongue-base / structural snorers | $25–$150 | Strong RCT |
| Nasal Dilator Strips | Nasal | 65% (nasal type) | Nasal / congestion snorers | $0.40/night | Strong |
| Nasal EPAP Valve | Nasal | 52% | Nasal + mild OSA | $20–$60 | Moderate |
| Tongue-Stabilizing Device (TSD) | Mouthpiece | 60% | Tongue-base snorers, denture wearers | $30–$80 | Moderate |
| Positional Sleep Trainer | Wearable | 74% (positional) | Positional snorers only | $60–$200 | Strong |
| Chin Strap | External | 30% | Mouth-open snorers only | $10–$30 | Weak |
| Smart Anti-Snore Pillow | Pillow | 45% | Positional + mild snorers | $100–$350 | Emerging |
| Throat Spray / Lubricant | Topical | <10% | Not recommended | $8–$20 | No Evidence |
| CPAP Machine | Pressure | 95%+ | Confirmed sleep apnea (OSA) | $500–$3,000 | Gold Standard |
A 2025 systematic review in the Journal of Sleep Research confirmed MADs reduced snoring frequency in 70% of users, increased deep sleep by an average of 18 minutes per night, and reduced snoring-related micro-arousals significantly. The key is fitting: a boil-and-bite MAD costs under $50 and should be the first device you try for tongue-base snoring before spending hundreds on custom dental devices.

06 / Real-World Case Studies — How 3 People Fixed Their Snoring
These three case studies represent the three most common snoring profiles we encounter. They’re anonymized composites drawn from reader submissions and community sleep forums — but the snoring types, interventions, and outcomes reflect patterns validated in clinical literature.
Case #1 — Mark, 47, Sales Manager, Chicago
BMI 31 · Neck 18.5″ · Drinks 2–3 glasses wine nightly · Back sleeper · Snoring since age 38
Mark’s wife had been sleeping in a separate room for 3 years. His snoring was loud enough to be heard through a closed door (measured at 68–72 dB on SnoreLab). He’d tried nasal strips, throat sprays, and a cheap mouthguard from Amazon with no improvement. What he hadn’t changed was his evening wine routine and his sleep position.
His intervention had three parts: he moved his last drink to 5+ hours before bed, placed a full-length body pillow to prevent supine sleep, and began a 15-minute throat exercise routine nightly. He lost 11 pounds over 8 weeks as a secondary lifestyle change.
“I didn’t believe exercises could do anything for snoring — it sounds absurd. But by week 4, my wife moved back into the bedroom. By week 8, she said I was basically silent. The wine timing change alone dropped my SnoreLab score by half.”
Case #2 — Sarah, 52, Teacher, Edinburgh
BMI 26 · Postmenopausal · Non-drinker · Side sleeper · Snoring started at menopause
Sarah’s snoring started suddenly at age 49, coinciding with the onset of menopause. This is extremely common — estrogen and progesterone help maintain airway muscle tone, and their decline during menopause dramatically increases snoring risk. By her mid-50s her snoring was waking her husband multiple times per night, and she was exhausted despite sleeping 8 hours.
Her GP ordered a home sleep apnea test that came back clear — no OSA. Her sleep specialist recommended a MAD mouthpiece, which she resisted for months before trying a $38 boil-and-bite model. Result: remarkable improvement within two weeks. She later moved to a custom dental MAD ($650) for better comfort on long-term wear.
“I kept thinking ‘I’m not overweight, I don’t drink, I sleep on my side — why am I snoring?’ Nobody told me menopause literally changes your airway muscle tone. The mouthpiece felt weird for the first three nights, then I stopped thinking about it — and the snoring stopped.”
Case #3 — Aiden, 34, Software Developer, New York
BMI 22 · Lean · Non-smoker · Seasonal allergies · Snoring Oct–May only
Aiden was baffled. He was 34, lean, non-smoker, almost never drank — and his girlfriend said he snored like “a freight train” from October through May. During summer months: nearly silent. The pattern was unmistakable once identified: his snoring was purely seasonal, driven by allergic rhinitis causing nighttime nasal congestion that forced him to mouth-breathe all night.
His fix was simple and inexpensive: daily non-drowsy antihistamine (cetirizine), Breathe Right nasal strips nightly, and a bedroom HEPA air purifier to remove airborne allergens. Total monthly cost: under $25. Total time to fix: three nights.
“I’d been spending money on all these mouthpieces and anti-snoring gadgets and nothing worked. It was my allergies the whole time. The nasal strips plus antihistamine fixed it in literally three days. Three days. I felt like an idiot for not figuring it out sooner.”
All three cases share one thing: the fix only worked once the correct root cause was identified. Mark’s nasal strips did nothing because his snoring was positional + alcohol-related. Sarah’s lifestyle changes did nothing because her cause was structural/hormonal. Aiden’s mouthpieces did nothing because his cause was allergic nasal obstruction. Identify first — then fix.
07 / Top Anti-Snoring Products on Amazon — Expert Picks 2026
These products are selected based on clinical evidence quality, Amazon rating consistency, and value-for-money. Each is matched to a specific snoring type so you’re not buying the wrong tool.

Breathe Right Extra Strength Nasal Strips (72-pack)
The most clinically studied nasal dilator strip available. Expands the nasal valve up to 38% more than decongestant spray. Drug-free, works same night. Best for allergy and congestion-driven snoring.
View on Amazon →
VitalSleep Anti-Snoring Mouthpiece — Adjustable MAD
Boil-and-bite custom fitting + micro-adjustment screw for precise jaw advancement. FDA cleared. Works for 70% of tongue-base snorers. Includes 1-year warranty and free replacements.
View on Amazon →Xtreme Comforts 7.5″ Wedge Pillow — Memory Foam
7.5-inch incline elevates head and torso — not just the neck — preventing soft tissue collapse. Also reduces acid reflux snoring. Machine-washable bamboo cover. Ships with 30-night trial.
View on Amazon →Levoit Core 300 HEPA Bedroom Air Purifier
H13 True HEPA filter captures 99.97% of allergens, dust mites, and pet dander. Quiet sleep mode (24dB). Covers 220 sq ft. Removes the airborne triggers that cause nighttime nasal congestion and allergy-driven snoring.
View on Amazon →Smart Nora — Contactless Anti-Snoring Device
Detects snoring sounds via bedside pebble, then quietly inflates an insert under your pillow to gently reposition your head — stimulating natural throat clearing. No mask, no mouthpiece. Works for most snoring types. Best non-invasive device for couples.
View on Amazon →Cushy Form Full-Length Body Pillow — Side Sleeping
Prevents rolling onto your back during sleep — the simplest and cheapest fix for positional snorers. 54-inch full-body length keeps spine and airway aligned. Washable cover included. Works the first night.
View on Amazon →08 / 3 Snoring Myths That Are Completely Wrong
These three myths are so widespread that they actively prevent people from fixing their snoring. Don’t let them delay your solution.
09 / When Snoring Is a Medical Emergency — Red Flags
Most snoring is benign and fixable at home. But these warning signs mean your snoring is a symptom of something more serious that requires immediate medical evaluation. Do not ignore these.
- Witnessed breathing pauses: Your partner notices you stop breathing for 10+ seconds during sleep, then gasp or choke awake — this is the textbook definition of obstructive sleep apnea.
- Excessive daytime sleepiness: You feel genuinely exhausted despite getting 7–9 hours of sleep — not just “a bit tired,” but unable to stay awake during meetings, while driving, or watching TV.
- Waking with headaches: Morning headaches (especially frontal headaches) are a classic sign of overnight hypoxia — low blood oxygen from repeated breathing obstructions.
- Neck circumference over 17″ (men) or 16″ (women): Combined with snoring, this is a strong independent predictor of OSA even without other symptoms.
- High blood pressure that’s hard to control: OSA is the most common secondary cause of treatment-resistant hypertension. If your BP medications aren’t working, ask about a sleep study.
- Snoring in a child: Childhood snoring, especially with mouth breathing and restless sleep, strongly suggests enlarged adenoids or tonsils and requires ENT evaluation — it can affect cognitive development if untreated.
- New snoring after 60: New-onset snoring in older adults requires evaluation because it can signal neurological changes, not just airway issues.

- Identify your snoring type using the decision flowchart above
- Remove alcohol within 3 hours of sleep tonight
- Set up a body pillow or tennis ball to prevent back sleeping
- Try nasal strips if you have any nasal congestion at all
- Download SnoreLab (free tier) to track your baseline snoring score
- Begin throat exercises — 15 minutes, every evening
- If any red flags apply, book a GP or sleep specialist appointment this week
10 / Frequently Asked Questions
Ready to Sleep in Silence Tonight?
Use our free Sleep Calculator to find your optimal bedtime, wake time, and sleep cycle — and discover if your snoring is affecting your deep sleep stages.
Try the Free Sleep Calculator →2. Camacho M et al. Myofunctional therapy to treat obstructive sleep apnea: a systematic review and meta-analysis. CHEST Journal, 2025.
3. Ravesloot MJL et al. The undervalued potential of positional therapy in position-dependent snoring and OSA. Sleep Medicine Reviews, 2025.
4. Sutherland K et al. Mandibular advancement splint effectiveness in snoring: RCT. Journal of Sleep Research, 2025.
5. Franklin KA et al. Snoring, pregnancy-induced hypertension, and growth retardation. Thorax.
6. Young T et al. The occurrence of sleep-disordered breathing among middle-aged adults. NEJM.
7. Peppard PE et al. Increased prevalence of sleep-disordered breathing in adults. American Journal of Epidemiology.
8. Stradling JR et al. Predictors and prevalence of obstructive sleep apnoea. Annals of Internal Medicine.
9. Deary V et al. Simple snoring: not quite so simple after all? Sleep Medicine Reviews.
10. Stuck BA et al. Diagnosis and treatment of snoring in adults. Deutsches Ärzteblatt International.
11. Lévy P et al. OSA syndrome. Nature Reviews Disease Primers.
12. Redline S et al. Sleep-disordered breathing and cardiovascular disease. American Journal of Respiratory and Critical Care Medicine.