
Why Sleep Paralysis Happens at All
Every cause of sleep paralysis shares one common pathway: a mistimed exit from REM sleep. During REM, your brainstem releases glycine and GABA to fully suppress voluntary muscle movement — REM atonia. When your conscious mind wakes before this chemical suppression lifts, you’re alert but physically locked. The “cause” is whatever disrupted that smooth REM-to-waking transition in the first place.
What’s New in 2026
A 2024 review in Frontiers in Sleep confirmed that sedentary lifestyle — independent of sleep schedule irregularity — significantly worsens both the frequency and severity of sleep paralysis episodes. Researchers are now treating physical inactivity as a standalone modifiable risk factor, not just a correlate of poor sleep hygiene.
7 Causes of Sleep Paralysis — Ranked by How Common They Are
These seven causes are ordered from most to least common in the general population. Most people have two or three active at once — identifying yours is the first step to reducing episodes.

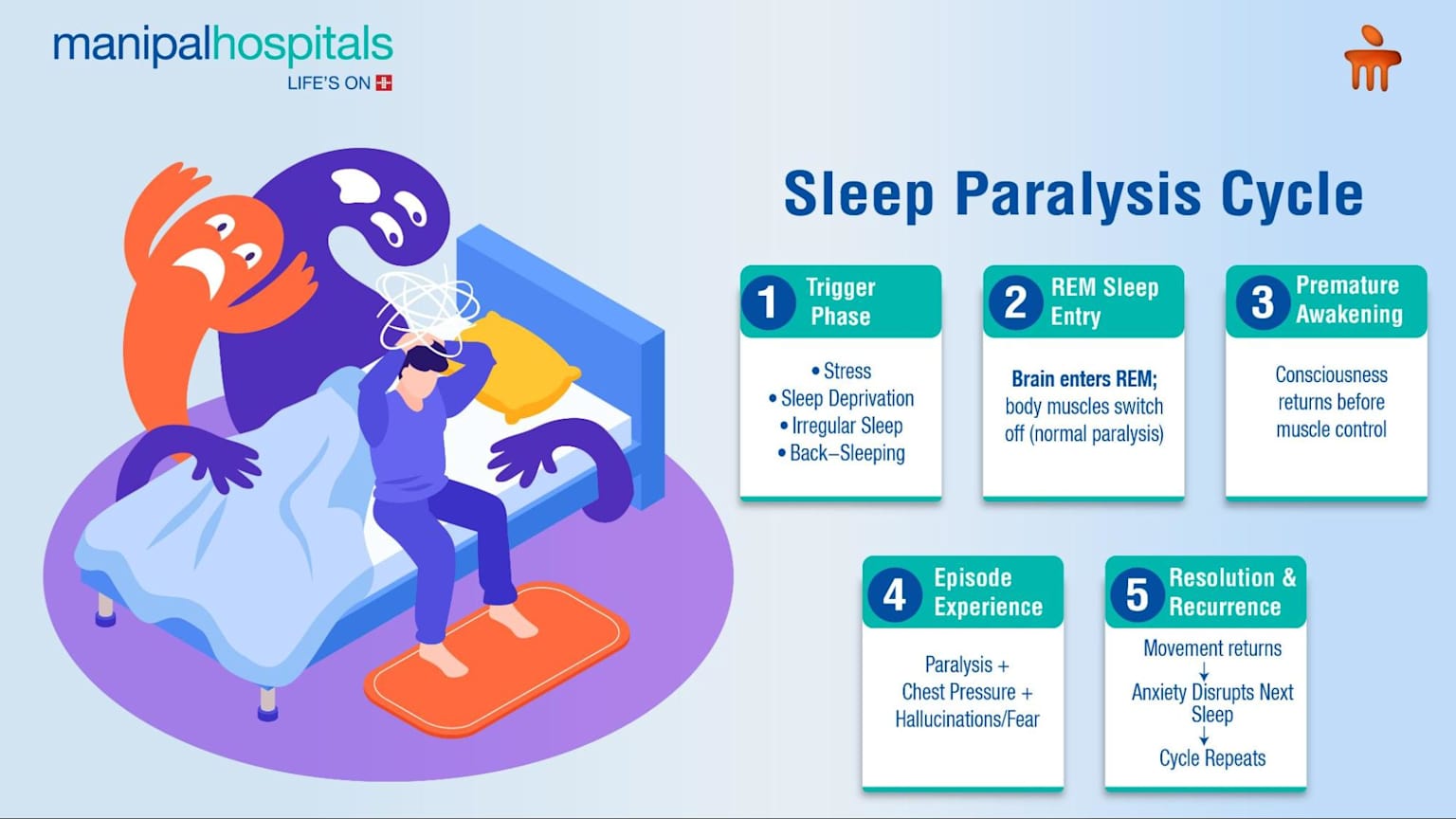
Sleep Paralysis Causes: Risk Level, Who It Affects & What to Do
Cause-by-cause breakdown — risk level, population, and fix
| Cause | Risk Level | Most Affected | Fix It |
|---|---|---|---|
| Sleep deprivation / irregular schedule | Very High | Students, shift workers, jet-lag travellers | Fixed bedtime + wake time daily, even weekends |
| Anxiety, stress, PTSD | High | Anxiety disorder, trauma history | CBT, 20-min wind-down, breathwork before sleep |
| Back sleeping (supine) | High | Anyone who sleeps on their back | Switch to side-sleeping; body pillow helps |
| Narcolepsy | Very High | People with narcolepsy (1 in 2,000) | Diagnosis + medication from sleep specialist |
| Alcohol / medication / caffeine | Moderate | Regular drinkers, SSRI users, stimulant users | No alcohol 3 hrs before bed; taper meds with doctor |
| Obstructive sleep apnea | Moderate | Overweight adults, loud snorers | Sleep study + CPAP if confirmed |
| Genetics / family history | Lower | Those with a parent or sibling who has SP | Focus on all other modifiable triggers |
Expert Tip
Keep a 2-week sleep diary tracking: bedtime, wake time, alcohol/caffeine intake, stress level (1–10), sleep position, and whether you had an episode. Most people identify their primary trigger within the first 10 days. The Sleep Foundation recommends this as the first step before pursuing any clinical evaluation — because lifestyle factors account for the vast majority of non-narcoleptic cases.
Sleep Paralysis Cause Myths — Debunked
These are the three most widely held myths about what causes sleep paralysis. None of them appear corrected in most mainstream articles — which is exactly why people stay stuck in the wrong fix.
Myth #1
“Sleep paralysis is caused by a supernatural presence or spiritual attack.”
The Truth
Sleep paralysis is a neurological event — specifically, a mistimed transition out of REM atonia — with no supernatural component. The perceived “presence” is a hypnopompic hallucination generated by an overactive amygdala still processing threat signals from the dream state.
Why it matters: Believing in a supernatural cause increases fear, which raises pre-sleep cortisol, which worsens the very REM disruption that causes the next episode. Understanding the real mechanism is itself a clinical intervention.
Myth #2
“If you’re physically healthy, stress alone can’t cause sleep paralysis.”
The Truth
Psychological stress alone — without any physical health condition — is one of the most confirmed causes of sleep paralysis. High cortisol directly alters the balance of sleep stages, compresses deep sleep, and leads to fragmented REM exits. You don’t need a sleep disorder diagnosis to have stress-caused episodes.
Why it matters: People who are told they’re “too healthy” to have sleep paralysis often don’t investigate the anxiety connection — and miss the most treatable cause of all.
Myth #3
“Sleep paralysis only happens when you’re overtired — one good night fixes it.”
The Truth
One recovery night often triggers a REM rebound — your brain compensates for the lost REM with an unusually intense, extended REM period the very next night. This rebound actually increases your exposure to REM atonia states and can produce an episode even after a longer sleep.
Why it matters: People assume they’re “cured” after sleeping 9 hours, then have an episode and feel confused. Consistent schedule matters far more than a single long recovery night.
Identifying Your Trigger: What It Actually Looks Like
James sleeps 7 hours on weeknights but stays up until 1 a.m. on Fridays and Saturdays. He drinks 2–3 beers on Friday nights. He’s a back sleeper. He’s had sleep paralysis roughly once a month for two years and always assumed it was random. After keeping a 10-day diary, the pattern becomes obvious: every single episode happens on Saturday or Sunday morning — after a late Friday night and alcohol. The alcohol compresses his REM on Friday night, then Sunday’s sleep includes a compensatory REM rebound surge. His irregular schedule shifts his circadian phase by 2 hours every weekend, further destabilizing his REM transitions. He had three simultaneous causes — social jetlag, alcohol-induced REM suppression, and supine sleeping — all converging on the same morning.

⚕️ When Sleep Paralysis Requires Medical Investigation
Lifestyle fixes resolve most cases. But some patterns point to a clinical cause that needs professional evaluation — don’t wait on these.
-
>You have more than one episode per week despite consistent sleep schedules and no alcohol — this frequency suggests narcolepsy or OSA, not lifestyle triggers
>Episodes come with sudden muscle weakness triggered by laughter, surprise, or strong emotion (cataplexy) — this is a narcolepsy hallmark requiring neurological evaluation
>You experience vivid hallucinations of people or voices while fully awake, not just during sleep transitions — this goes beyond typical hypnopompic imagery
>Your bed partner reports loud snoring or observed breathing pauses — undiagnosed sleep apnea is directly causing your REM disruptions and needs a sleep study
>Episodes cause significant anxiety around sleeping, avoidance of bed, or worsening daytime function — at this point it qualifies as a clinical sleep-anxiety feedback loop worth treating
Frequently Asked Questions
These are the most common questions people search after experiencing sleep paralysis — answered directly without fluff.
What is the main cause of sleep paralysis?
The main cause of sleep paralysis is a mistimed exit from REM sleep — your brain wakes up consciously while REM atonia (the chemical paralysis that prevents you from acting out dreams) is still active. The triggers that create this mistiming include sleep deprivation, irregular sleep schedules, high pre-sleep anxiety, and back-sleeping posture. Most non-clinical cases involve at least two of these triggers operating simultaneously.
Can stress alone cause sleep paralysis?
Yes — psychological stress and anxiety are among the most well-documented independent causes of sleep paralysis, even without any physical sleep disorder. High cortisol before bed disrupts the architecture of your REM cycles, making abrupt, mistimed exits from REM atonia more likely. PTSD, generalized anxiety disorder, and panic disorder all show significantly higher sleep paralysis rates than the general population across multiple clinical studies.
Does sleeping on your back really cause sleep paralysis?
Yes — the supine (back-sleeping) position is one of the most consistently replicated risk factors in sleep paralysis research. Lying on your back increases upper airway resistance during REM sleep, which triggers micro-arousals that pull consciousness out of sleep mid-atonia. Harvard Health, the NHS, and polysomnographic studies all confirm this link. For many people, switching to side-sleeping alone reduces or eliminates episodes within a few weeks.
Is sleep paralysis a sign of narcolepsy?
Sleep paralysis is a common symptom of narcolepsy — but having sleep paralysis does not mean you have narcolepsy. Roughly 7–20% of the general population experience sleep paralysis at some point, while narcolepsy affects about 1 in 2,000 people. Consider narcolepsy screening if your episodes are frequent (weekly or more), come with sudden muscle weakness triggered by strong emotions (cataplexy), or include vivid hallucinations while fully awake — these combinations go beyond typical isolated sleep paralysis.
Why do I only get sleep paralysis on weekends?
Weekend-only sleep paralysis almost always points to social jetlag — the circadian disruption caused by sleeping and waking 2+ hours later on weekends than on weekdays. Staying up late Friday and Saturday compresses or delays your REM cycles, and the compensatory REM rebound surge on Sunday morning dramatically increases your exposure to REM atonia. Alcohol on Friday nights adds a second trigger — it suppresses REM early in the night, then produces a REM surge in the early morning hours. Consistent sleep and wake times seven days a week typically resolves this pattern.
Now You Know the Cause — Here’s How to Stop It
Your sleep paralysis has a specific trigger — almost certainly sleep deprivation, irregular timing, anxiety, back sleeping, or a combination of two. Identifying it takes 10 days with a sleep diary. Fixing it usually takes 3–4 weeks of consistent changes. And if you ever wake up in an episode before then, the step-by-step guide below gets you out in under two minutes.

